Medik Blog
What Is The Trendelenburg Position?
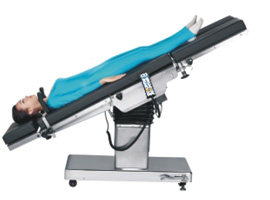 | In the Trendelenburg position, the body is laid supine, or flat on the back on a 15–30 degree incline with the feet elevated above the head. |
When to use The Trendelenburg Position?
The Trendelenburg position is used in surgery, especially of the abdomen and genitourinary system. It allows better access to the pelvic organs as gravity pulls the intra-abdominal organs away from the pelvis. Evidence does not support its use in hypovolaemic shock, with concerns for negative effects on the lungs and brain.
Considerations For Trendelenburg Position
When positioning a patient in Trendelenburg, surgical staff should consider various factors, including risk factors, the potential for injury, and clinical recommendations for repositioning.
* Brachial Plexus Neuropathy – The approximation of the clavicle and first rid threatens compression of the subclavian vessels and brachial plexus. Shoulder braces are causal to brachial plexus neuropathy: Gravity pulls the patient’s weight against shoulder braces, causing the shoulders to yield to pressure, and body mass slides between the braces.
* Perioperative complications from extreme Trendelenburg positioning – Keeping a patient in Trendelenburg for a long period of time may lead to a risk of various injuries, including ocular trauma due to increased blood pressure in the head including corneal abrasion, retinal detachment, ischemic optic neuropathy, as well as respiratory distress.
* Clinical recommendations for repositioning patients – Steep Trendelenburg patient position present risk for intraoperative injury. Injury prevention begins with awareness. Several mitigations can be deployed including; anesthesia administered crystalloids to reduce the risk for neural edema, surgeons should use the least amount of pneumoperitoneum needed for the surgery, and using the least amount of Trendelenburg needed for the procedure. The nursing team should monitor the patient's position. Second timeouts involving checking patient positioning and making adjustments based on the patient's physiological and physical status have been proposed for cases taking longer than 4 hours. It is standard for the nursing staff to check the safety of patient position during the case every hour when feasible. Introducing pauses for positioning checks and relieving Trendelenburg for even brief periods of time can reduce the risk for the most common injuries sustained while patients are in this position.
Trendelenburg Position Vs. Reverse Trendelenburg Position
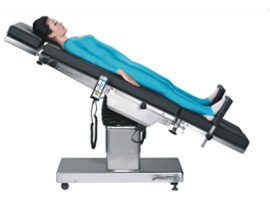 | In the Trendelenburg position, the body is laid supine, or flat on the back on a 15–30 degree incline with the feet elevated above the head. The reverse Trendelenburg position, similarly, places the body supine on an incline but with the head now being elevated. Reverse Trendelenburg position is used for laparoscopic surgeries including gallbladder, biliary tract, and stomach procedures, as well as head and neck surgeries. Most recently, the Reverse Trendelenburg position has been used in minimally invasive glaucoma surgery, also known as MIGS. This position is commonly used for a superior sitting surgeon that uses a combination of downward patient tilt, of approximately 30 to 35 degrees, microscope tilt towards themselves at the same angle, and an intraoperative gonio lens or prisms that allows them to visualise the inferior trabecular meshwork. |
*PLEASE NOTE: We are healthcare equipment suppliers, and therefore are not qualified to give any clinical or medical advice.*
References
1.Ostrow, CL (May 1997). "Use of the Trendelenburg position by critical care nurses: Trendelenburg survey". American Journal of Critical Care. 6 (3): 172–6.
2. Johnson, S; Henderson, SO (2004). Canadian Journal of Emergency Medicine. 6(1): 48–9. doi:10.1017/s1481803500008915. PMID 17433146.
3. Zillioux JM, Krupski TL. Patient positioning during minimally invasive surgery: what is current best practice? Robot Surg. 2017;4:69-76. Published 2017 Jul 14. doi:10.2147/RSRR.S115239